Research - (2021) Volume 9, Issue 11
Influence of Material Layer Deposition Thickness, Span Length of Prosthesis, and type of Laser on the Surface Marginal fit of Different Surfaces of DMLS copings Fabricated using 3 Different DMLS Printing Machines
Harsh Kasabwala1*, Deepak Nallaswamy2 and Subhashree R1
*Correspondence: Harsh Kasabwala, Department of Prosthodontics, Saveetha Dental College and Hospitals, Saveetha Institute of Medical and Technical Sciences, Saveetha University, Chennai, India, Email:
Abstract
Background: Metal-ceramic restorations are frequently made using laser sintering. The sintering process' layer thickness may have an impact on restoration adaptation. However, there is little information about its impact. Aim: The goal of this in vitro experiment was to compare the marginal adaptation of laser-sintered cobalt-chromium long span bridges and single crown frameworks made on different DMLS machines. Methods: Tooth preparation was carried out on a typhodont teeth set from 14-22 and for 16. The dies were scanned and the samples were designed using 3 Shape software. The samples were then laser sintered using 3 different DMLS machines. Sample size consisted of 6 samples for the long span framework and 6 samples for the single crown framework per machine. Marginal accuracy was evaluated at 6 different points (mesiobuccal, buccal, distobuccal, mesiopalatal, palatal and distoplatal surface). The microscopic evaluation was carried out using a stereomicroscope. The discrepancy and internal fit values were recorded and tabulated. Spss version 20 software was used to carry out statistical analysis. Descriptive ANOVA test followed by Benferroni test was used to evaluate the statistical significance. Results: The proximal surfaces showed higher discrepancy levels as compared to the other surfaces. The mean values of the marginal discrepancy values were comparatively higher on the proximal surfaces (mesiobuccal, mesiopalatal, distobuccal and distopalatal points) as compared to the buccal and palatal surfaces (buccal and palatal points). There was a statistically significant difference in the marginal discrepancy values of the dmls copings fabricated using different DMLS printing machines on the mesiopalatal, distopalatal and distobuccal surfaces (P value <0.05). Conclusions: Best marginal fit values were achieved with the EOS machine suggesting that the metal deposition layer thickness as well as the type of laser did have a significant impact on the marginal fit of the prosthesis. The proximal surfaces showed higher discrepancy levels as compared to the other surfaces again questioning the accuracy of the scanner, designing software and the DMLS machines. The span length did have an impact on the overall fit of the prosthesis suggesting that there might be errors incorporated during the scanning or during the metal printing.
Keywords
DMLS, Coings, Marginal fit, Span length, Metal printing, DMLS printers
Introduction
The adaptation of restorations is closely linked to the longterm clinical success of fixed prostheses. Cement dissolution, plaque accumulation and bacterial growth, as well as secondary caries or periodontal disorders, are all triggered by increased marginal discrepancy [1-3]. As a result, optimal marginal and internal adaptation between the restoration and the prepared tooth structure should be established [3-5]. Although authors disagree on what constitutes a clinically acceptable marginal discrepancy value, most agree that values greater than 120 μm are not clinically acceptable [6-8]. Furthermore, there is no agreement on the ideal cement film thickness [8,9]. Material-specific recommendations have been made in previous studies [8-11]. Marginal discrepancy can be assessed using a variety of methods, the most common of which are direct microscopic evaluation, sectioning, and the replica method [11-13].
The excellent mechanical properties of metal-ceramic restoration have continued the popularity and success of this treatment option [14]. For many years, the traditional lost-wax method has been used to fabricate metal-ceramic restorations; however, this method has some drawbacks, including multiple technique-sensitive steps and the development of casting imperfections [1]. Because of their high accuracy and consistent quality, computer-aided design and manufacturing (CAD-CAM) systems have become increasingly popular in recent years [15,16]. Subtractive manufacturing systems (such as milling) and additive manufacturing systems (such as laser sintering) are the two types of CAD-CAM systems currently used in dentistry [15-18].
Metal-based prostheses are increasingly being made with laser sintering systems. These systems use a laser source to consolidate powdered material layer by layer to convert CAD data into 3-dimensional (3D) complex structures [19]. Direct metal laser sintering (DMLS), which involves partial melting of metal powders, or direct metal laser melting (DMLM), which involves complete melting of metal powders, can be used to sinter metal powder [18,20]. The complete melting of metal powders results in a high-density structure (approximately 99.8 percent).
For dental applications, there are several DMLS and DMLM machines available, including the EOSINT M270; EOS GmbH (DMLS), M1; Concept Laser GmbH (DMLM), and MYSINT 100; Sisma SpA (DMLM), Shining 3D (DMLS), OR LASER (DMLS), and others [21]. The thickness of the sintering layer and the power consumption of the machine determines the mechanical properties of the metal structures produced during the laser sintering process. However, dental laboratories are primarily responsible for determining this parameter [22,23]. Reducing the layer thickness improves mechanical properties, while increasing it beyond a certain point causes major issues like poor surface finish, decreased accuracy, and decreased mechanical properties. The sintering layer thickness can be adjusted between 20 and 100 μm, but the capacity of laser sintering machines may limit this [24,25]. This in vitro study compared the marginal and internal adaptation of laser-sintered cobalt-chromium (Co-Cr) frameworks with layer thicknesses of 20 and 100 μm fabricated using three different DMLS machines. According to the study hypothesis, metal frameworks sintered with a layer thickness of 20-50 μm showed improved marginal and internal adaptation.
Methods
Study setting
The present study was carried out as an In Vitro study under a university setting in Saveeta dental College Chennai. The ethical approval was given by the research department Saveetha institute of medical and technical sciences Chennai (SIMATS). (IHEC/SCD/PROS-SDC 1803/04). The sample size was calculated using G power software.
Sample size calculation
The studies carried out by Papadiochou et al, James et al and Park et al were used as parent studies out of which the sample size was calculated using g power software [26-28]. A total of 126 samples were estimated according to the software readings which comprised of 18 six unit bridges (6 per machine) and 18 single crowns (6 per machine). The three machines used for the comparison study were EOS M 100, Shining 3D EP-M 100T and OR laser Creator machine.
Die preparation
A typodont teeth set was used to prepare the dies. Tooth preparation was carried out using a straight flat and diamond bur. Teeth which were prepared comprised of 14-22 and 16. Precautions were taken to avoid creation of any kind of undercuts while doing the tooth preparation. A smooth shoulder finish line was provided to all the prepared teeth. The prepared acrylic teeth were then finished with a yellow band finishing bur.
Scanning of The Prepared Model
Scanning of the dies separately
The prepared acrylic teeth were then removed from the typodont and were scanned separately without the model. This was done to accurately scan and record the finish margins of the teeth and all the unreachable surfaces.
Scanning of the model
The typodont model was then scanned without the acrylic teeth. This step was done so that the prepared teeth could be aligned with the model.
Superimposition of dies to the model
Finally the prepared acrylic teeth what is superimposed with the model both of which were scanned separately. The two scans were aligned by marking aligning points on the MEDIT software. This final scan was then exported for designing the copings.
Designing of the copings
The copings were designed in the 3-shape software. The procedure involved in designing consisted of setting of the insertion direction of the prosthesis, marking of the finish line and finally morphing of the copings which were generated.
STL file generation
The design that was made digitally was converted into an STL format and was exported for printing using the three different machines.
DMLS machines used and their features
The three machines used for the comparison study were EOS M 100, Shining 3D EP-M 100T and OR laser Creator machine.
Layer thickness
The layer thickness of the EOS machine was between 20 to 40 μm whereas the layer thickness for the Shining 3D machine was between 50 to 80 μm and that for the OR laser machine was between 50-100 μm. The layer thickness for the EOS machine was the least suggesting that the metal micro-particles were arranged in a more compact fashion for the EOS machine.
Type of laser used
All the three machines used Ytterbium laser in order to carry out the sintering process.
Type of gas inlet
All the 3 machines used argon inert gas while carrying out the printing procedure. The inert gas helps in enhancing the overall productivity of the printed prosthesis.
Printing procedure
The first step involved loading of the STL format into the DMLS machine software. This was followed by nesting of the prosthesis followed by providing support sprews.
The printing platform was then cleaned and set up for the procedure. Precautions were taken to make sure that the printing platform did not have any kind of old material or scratches to avoid failures. Finally the printing procedure was started wherein the recoater arm added the material layer by layer till the final prosthesis was built. Precautions were taken to avoid pausing procedure as it could have led to inaccuracies.
Post printing procedures
Once the printing was completed the prosthesis was then heat treated following which the sprews were carefully cut with a metal cutting bur. Precautions were taken to avoid touching the metal cutting bur on the surface of the prosthesis. Two of the samples fabricated using OR laser machine was inadvertently damaged with the bur rendering them any useful for the surface roughness study.
Evaluation of Marginal Fit
Apparatus
The marginal fit was evaluated using a Lawrence and Mayo stereo microscope at the optical zooming of 80x. A Matt black background was used while examining the samples to avoid any kind of reflection.
Procedure followed
The marginal discrepancy evaluation was carried out at six different points on the prepared tooth namely mesiobuccal, buccal, distobuccal, mesiolingual, lingual and distolingual. The stereo microscope was focused at each point and the discrepancy in micrometres was calculated.
The software used for the calculation was Magvision. The distance between the margin of the prosthesis and the finish line was calculated for each sample. A total of 756 points were evaluated and the readings were tabulated.
Tabulation and statistical analysis done
The tabulation was done based on the type of surface that is being examined and the tooth which is being evaluated. SPSS version 20 software was used for tabulation and for descriptive statistics. The means for each surface discrepancy was calculated for every tooth. ANOVA statistical test was done to compare means and to find out the statistical differences between the different samples.
Statistical analysis
SPSS version 20 software was used for tabulation and for carrying out the statistics. Descriptive statistics were done to evaluate the mean and standard deviation for all the three parameters. ANOVA statistical test was done to compare means and to find out the statistical differences between the different samples or all the parameters.
Independent variables included Laser used by the machine, Gas inlet for the machine, Metal used for printing, Software used to evaluate the marginal and internal discrepancy, Magnification used to focus on the surface is being examined, Typodont model Dependent variables included; Marginal discrepancy, internal fit, surface roughness.
Results
Distopalatal surface
The overall mean values for the distopalatal surface marginal discrepancy were comparatively lower for the EOS machine followed by Shining 3d and finally maximum for OR laser. There was a significant difference in the marginal discrepancy values of the 3 groups on the distopalatal surface concerning the tooth number 13,12,11,22 and 16 after one way ANOVA test (P values<0.05). Based on the Post Hoc analysis using Bonferroni test, there was a statistical difference between the marginal discrepancy values of the coping fabricated using Shining 3d and EOS machine concerning the toothnumber13 (p value<0.05). Similarly, there was a statistical difference between the marginal discrepancy values of the copings fabricated using OR laser and EOS machine concerning the tooth number 22, 11 (p value<0.05). There was no statistical difference when the discrepancy values of Shining 3d was compared to OR laser machine.
Mesiobuccal surface
The overall mean values for the mesiobuccal surface marginal discrepancy were comparatively lower for the EOS machine followed by Shining 3d and finally maximum for OR laser. There was a significant difference in the marginal discrepancy values of the 3 groups on the mesiobuccal surface concerning the tooth number 14,12,11,21,22 and 16 after one way ANOVA test (P values<0.05). Based on the Post Hoc analysis using Bonferroni test, there was a statistical difference between the marginal discrepancy values of the coping fabricated using Shining 3d and OR laser machine concerning the tooth number 12,11,21,16 and14 (p value<0.05). Similarly there was a statistical difference between the marginal discrepancy values of the copings fabricated using OR laser and EOS machine concerning the tooth number 12, 11,21,22,16 and14 (p value<0.05). There was no statistical difference when the discrepancy values of Shining 3d were compared to EOS machine.
Buccal surface
The overall mean values for the buccal surface marginal discrepancy were comparatively lower for the EOS machine followed by Shining 3d and finally maximum for OR laser. There was a significant difference in the marginal discrepancy values of the 3 groups on the buccal surface concerning the tooth number 14, 12, 21 and 16 (P values<0.05). Based on the Post Hoc analysis using Bonferroni test, there was a statistical difference between the marginal discrepancy values of the coping fabricated using Shining 3d and OR laser machine concerning the tooth number 14, 12, 21and 16 (p value<0.05). Similarly, there was a statistical difference between the marginal discrepancy values of the copings fabricated using OR laser and EOS machine concerning the tooth number 14, 12, 21and16 (p value<0.05). There was no statistical difference when the discrepancy values of Shining 3d were compared to EOS machine.
Distobuccal surface
The overall mean values for the distobuccal surface marginal discrepancy were comparatively lower for the EOS machine followed by Shining 3d and finally maximum for OR laser. There was a significant difference in the marginal discrepancy values of the 3 groups on the distobuccal surface concerning the tooth number 11, 21, 22 and 16 (P values<0.05). Based on the Post Hoc analysis using Bonferroni test, there was a statistical difference between the marginal discrepancy values of the coping fabricated using Shining 3d and OR laser machine concerning the tooth number 22 and 16 (p value<0.05). Similarly, there was a statistical difference between the marginal discrepancy values of the copings fabricated using OR laser and EOS machine concerning the tooth number 11, 21, 22 and16 (p value<0.05). There was no statistical difference when the discrepancy values of Shining 3d were compared to EOS machine.
Mesiopalatal surface
The overall mean values for the mesiopalatal surface marginal discrepancy were comparatively lower for the EOS machine followed by Shining 3d and finally maximum for OR laser. There was a significant difference in the marginal discrepancy values of the 3 groups on the mesiopalatal surface concerning the tooth number 14 and 11(P values<0.05). Based on the Post Hoc analysis using Bonferroni test, there was a statistical difference between the marginal discrepancy values of the coping fabricated using Shining 3d and OR laser machine concerning the tooth number 11 (p value<0.05). Similarly there was a statistical difference between the marginal discrepancy values of the copings fabricated using OR laser and EOS machine concerning the tooth number 11(p value<0.05). There was a statistical difference between the marginal discrepancy values of the copings fabricated using Shining 3d and EOS machine concerning the tooth number 14.
Palatal surface
The overall mean values for the palatal surface marginal discrepancy were comparatively lower for the EOS machine followed by Shining 3d and finally maximum for OR laser. There was a significant difference in the marginal discrepancy values of the 3 groups on the palatal surface concerning the tooth number 14, 12, 11and 22(P values<0.05). Based on the Post Hoc analysis using Bonferroni test, there was a statistical difference between the marginal discrepancy values of the coping fabricated using Shining 3d and OR laser machine concerning the tooth number 12 and11 (p value<0.05). Similarly, there was a statistical difference between the marginal discrepancy values of the copings fabricated using OR laser and EOS machine concerning the tooth number 22, 11, 12 and 14 (p value<0.05). There was no statistical difference when the discrepancy values of Shining 3d were compared to EOS machine (Table 1 and Figures 1 to Figure 4).
| Dependent variable | (I) Machines | (J) Machines | Mean difference (I-J) | Std. Error | Sig. |
|---|---|---|---|---|---|
| MESIO BUCCAL SURFACE | |||||
| 13 | OR Laser | Shining 3D | 0.07667* | 0.025 | 0.02 |
| EOS | 0.10667* | 0.025 | 0.002 | ||
| 12 | OR Laser | Shining 3D | 0.08667* | 0.01409 | 0 |
| EOS | 0.09667* | 0.01409 | 0 | ||
| 11 | OR Laser | Shining 3D | 0.11667* | 0.02936 | 0.003 |
| EOS | 0.12000* | 0.02936 | 0.003 | ||
| 21 | Shining 3D | EOS | 0.08667* | 0.01893 | 0.001 |
| OR Laser | -0.06667* | 0.01893 | 0.008 | ||
| 16 | OR Laser | Shining 3D | 0.07000* | 0.02087 | 0.011 |
| EOS | 0.09333* | 0.02087 | 0.001 | ||
| 14 | Shining 3D | OR Laser | -0.07000* | 0.02087 | 0.011 |
| Buccal surface | |||||
| 14 | OR Laser | Shining 3D | 0.04000* | 0.00989 | 0.003 |
| EOS | 0.04667* | 0.00989 | 0.001 | ||
| 13 | OR Laser | Shining 3D | 0.10000* | 0.0259 | 0.004 |
| EOS | 0.17600* | 0.0259 | 0 | ||
| 12 | OR Laser | Shining 3D | 0.10000* | 0.0259 | 0.004 |
| EOS | 0.17600* | 0.0259 | 0 | ||
| 21 | OR Laser | Shining 3D | 0.07000* | 0.01713 | 0.003 |
| EOS | 0.08000* | 0.01713 | 0.001 | ||
| 22 | EOS | 0.10000* | 0.03412 | 0.026 | |
| 16 | OR Laser | Shining 3D | 0.03000* | 0.0073 | 0.003 |
| EOS | 0.03333* | 0.0073 | 0.001 | ||
| Distobuccal surface | |||||
| 11 | OR Laser | Shining 3D | 0.04333* | 0.01559 | 0.035 |
| 21 | OR Laser | Shining 3D | 0.08667* | 0.02238 | 0.004 |
| EOS | 0.08667* | 0.02238 | 0.004 | ||
| 22 | OR Laser | Shining 3D | 0.09667* | 0.02786 | 0.009 |
| EOS | 0.12667* | 0.02786 | 0.001 | ||
| 16 | OR Laser | Shining 3D | 0.06000* | 0.01549 | 0.004 |
| EOS | 0.07333* | 0.01549 | 0.001 | ||
| Mesio palatal surface | |||||
| 13 | OR Laser | EOS | 0.06000* | 0.01955 | 0.02 |
| 12 | Shining 3D | OR Laser | -0.06000* | 0.01955 | 0.02 |
| EOS | Shining 3D | 0.04333* | 0.01398 | 0.019 | |
| 11 | Shining 3D | OR Laser | -0.06000* | 0.01398 | 0.002 |
| Palatal surface | |||||
| 14 | OR Laser | Shining 3D | -0.00667* | 0.00172 | 0.004 |
| EOS | -0.00667* | 0.00172 | 0.004 | ||
| OR Laser | 0.00667* | 0.00172 | 0.004 | ||
| 12 | OR Laser | Shining 3D | 0.05667* | 0.01909 | 0.024 |
| EOS | 0.08000* | 0.01909 | 0.002 | ||
| 11 | OR Laser | Shining 3D | 0.02667* | 0.00689 | 0.004 |
| EOS | 0.02667* | 0.00689 | 0.004 | ||
| 22 | OR Laser | EOS | 0.12000* | 0.0391 | 0.02 |
| Distopalatal | |||||
| 13 | Shining 3D | EOS | 0.08333* | 0.0305 | 0.039 |
| 12 | OR Laser | EOS | 0.06667* | 0.02198 | 0.022 |
| 11 | OR Laser | EOS | 0.06000* | 0.01738 | 0.009 |
| 22 | OR Laser | EOS | 0.08667* | 0.027 | 0.015 |
| 16 | Shining 3D | EOS | 0.15333* | 0.05847 | 0.048 |
Table 1: Table showing the mean difference, standard error and significance values of the marginal discrepancies of DMLS copings fabricated using 3 different DMLS printing machines.
Figure 1: Pictorial representation of the three machines used to fabricated the dmls prosthesis (EOS M 100, Shining 3D EP-M 100T and OR laser Creator machine).
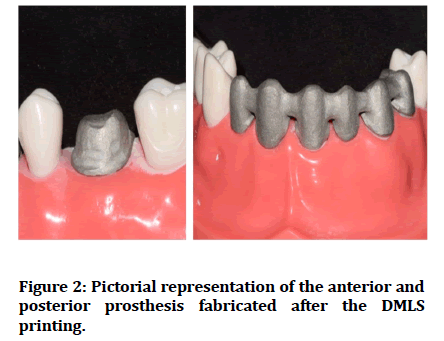
Figure 2:Pictorial representation of the anterior and posterior prosthesis fabricated after the DMLS printing.
Figure 3:Pictorial representation of the process of steriomicroscopic evaluation of the dmls copings.
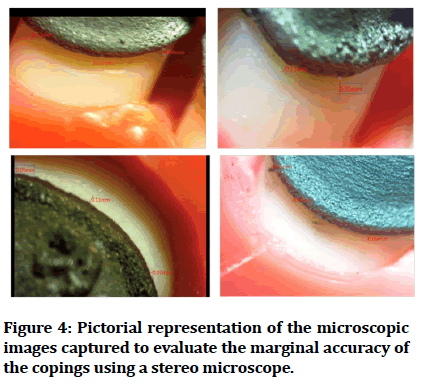
Figure 4:Pictorial representation of the microscopic images captured to evaluate the marginal accuracy of the copings using a stereo microscope.
Discussion
Previous laser sintering machines could handle layer thicknesses ranging from 50 to 80 mm. For dental applications, laser sintering systems with a layer thickness of approximately 20 mm have been introduce [29,30]. The depth of laser penetration is a critical factor in evaluating marginal discrepancy. It is more difficult to fully melt a thicker layer of powder, and unconsolidated sections between the layers can weaken the structure. As a result, the sintering layer thickness can influence the final product's consistency and dimensional properties [29–31]. Beyond a certain stage, increasing the sintering layer thickness reduces process accuracy and degrades surface finish, while decreasing the layer thickness by up to 20 mm improves process accu1racy. However, reducing the layer thickness to less than 20 mm can cause the structure to become more porous, and reducing the layer thickness typically increases the manufacturing time [23,18].
There have been very few studies that have evaluated the marginal accuracy and internal fit of dmls copings [32-34]. Additionally, there haven’t been any studies that have compared the efficiency of different DMLS machines based on the marginal and internal fit. In the current study the overall marginal discrepancy when evaluated for the 3 DMLS machines favoured the EOS machine as it showed the lowest discrepancy values. It was closely followed by the Shining 3D machine and finally the OR Laser machine which showed the maximum marginal discrepancy. The possible explanation for this could be the minimal metal layer thickness used by the EOS machine. Additionally, it can also be hypothesized that EOS machine showed comparatively better accuracy as the quality of laser and the power consumption could be superior to the other 2 machines. The EOS fulfilled all the required criteria for a perfect dmls machine be it in terms of layer thickness or power consumption. There have been only a handful number of studies which have evaluated the influence of layer thickness on the overall accuracy of the laser sintered prosthesis. Previous literature has shown no significant difference in the marginal accuracy of metal frameworks fabricated using different layer thickness (25microns, 50microns) during the printing process [29].
Similarly previous studies done on commercial metal fabrication using Selective laser melting and Stereolithography have proved the fact that lower the layer thickness of the material better is the accuracy and lower is the dimensional instability of the final product [34–37]. For determining marginal discrepancy, direct microscopy and sectioning are widely used [38,8]. Direct microscopy is a simple, fast, and repeatable process, but it is less accurate. Sectioning, on the other hand, is a difficult process that yields sensitive results. The drawback in the current study was the use of only stereo microscopy for evaluation of the marginal discrepancy which could be a bias as it is not perfectly accurate.
There haven’t been any studies that have evaluated the influence of prosthesis span length on the accuracy and marginal fit of DMLS fabricated prosthesis. Change in span length has shown to have a significant effect on marginal and internal fit in studies carried out on zirconia prosthesis [39]. The mean value of marginal fit in the single or four-unit fixed partial denture groups was within clinically reasonable limits. However, some margins in the 6-unit sample had values that were outside of the clinically appropriate range. Also, the curved anterior frameworks especially the ones crossing the midline have shown to have a significant impact on the marginal and internal fit of the prosthesis [40]. This suggested that increasing the span length could potentially reduce the fit of the prosthesis.
The results procured in the current study were consistent with the previously done studies as the long span framework and specifically the bilaterally distal abutments showed higher discrepancy values. The single molar crown showed comparatively less marginal discrepancy values as compared to the long span prosthesis. Another reason for the discrepancy in the long span frameworks especially the ones crossing the midline could be the inaccuracies incorporated in the scan due to the stitching algorithm. These inaccuracies would be reflected in the prosthesis in the form of marginal discrepancies [40–42]. These findings were also reflected in the current study as prepared cast was also scanned using a lab scanner.
The digitally designed prosthesis has shown to be more accurate in terms of overall marginal accuracy when compared to the conventionally fabricated ones but digital designs also have a few limitations [41–44]. The current study reflects that the digitally designs DMLS copings showed more discrepancies especially on the proximal surfaces. This result is in accordance with the one seen in a few previous studies wherein the buccal and lingual / palatal surfaces showed better marginal fit as compared to the proximal surfaces [32]. The possible reason for this could be the inability of the either the scanner to record the proximal surfaces accurately or the designing software to accurately detect the proximal marginal finish lines. There is also a possibility to that the DMLS machines are not quite capable to accurately replicate the margins on the proximal surfaces. There could be multiple explanations for these results, it is necessary to conduct more studies in this perspective to accurately pinpoint the root cause for the same. All the samples be it for marginal or internal fit were evaluated under stereomicroscope, which is not considered as the gold standard.
Only 3 machines were evaluated hence a generalized conclusive statement cannot be made for all the DMLS machinery. Additional research in terms of mechanical bond strength of dmls copings with ceramic, flexural strength and long-term survival of copings fabricated with various DMLS machines should be encouraged. Additionally, the microstructural and mechanical properties of the metal structures, on the other hand, were not assessed in this analysis. As a result, further research into the effects of different DMLS printing machines on laser-sintered restorations is required.
Conclusion
Different DMLS machines did have a significant influence on the marginal. Best marginal fit values were achieved with the EOS machine suggesting that the metal deposition layer thickness as well as the type of laser did have a significant impact on the marginal fit of the prosthesis. The proximal surfaces showed higher discrepancy levels as compared to the other surfaces again questioning the accuracy of the scanner, designing software and the DMLS machines. The span length did have an impact on the overall fit of the prosthesis suggesting that there might be errors incorporated during the scanning or during the metal printing. Based on the overall evaluation the EOS followed by Shining 3D machine showed quite promising results in terms of marginal and internal fit as most of their discrepancy readings were within clinically acceptable limits.
Acknowledgement
All involved authors make NO further acknowledgements.
Funding
Self.
Conflict of Interest
All involved authors declare no potential conflict of interest.
Ethical Approval
(IHEC/SCD/PROS-SDC 1803/04).
References
- Willer J, Rossbach A, Weber HP. Computer -assisted milling of dental restorations using a new CAD/CAM data acquisition system. J Prosthet Dent 1998; 80:346–53.
- Johnson R, Verrett R, Haney S, et al. Marginal gap of milled versus cast gold restorations. J Prosthodont 2017; 26:56–63.
- Park JM, Hong YS, Park EJ, et al. Clinical evaluations of cast gold alloy, machinable zirconia, and semiprecious alloy crowns: A multicenter study. J Prosthetic Dent 2016; 115:684-91.
- Kocaagaoglu H, Kilinç HI, Albayrak H, et al. In vitro evaluation of marginal, axial, and occlusal discrepancies in metal ceramic restorations produced with new technologies. J Prosthet Dent 2016; 116:368–74.
- Kokubo Y, Tsumita M, Kano T, et al. Clinical marginal and internal gaps of zirconia all ceramic crowns. J Prosthodont Res 2011; 55:40–43.
- Beuer F, Aggstaller H, Edelhoff D, et al. Marginal and internal fits of fixed dental prostheses zirconia retainers. Dent Mater 2009; 25:94–102.
- Kim KB, Kim JH, Kim WC, et al. Evaluation of the marginal and internal gap of metal-ceramic crown fabricated with a selective laser sintering technology: Two-and three-dimensional replica techniques. J Adv Prosthodont 2013; 5:179-86.
- Lopez-Suarez C, Gonzalo E, Pelaez J, et al. Marginal vertical discrepancies of monolithic and veneered zirconia and metal-ceramic three-unit posterior fixed dental prostheses. Int J Prosthod 2016; 29:256-8.
- Hickel R, Dasch W, Mehl A, et al. CAD/CAM fillings of the future? Int Dent J 1997; 47:247–58.
- Wu JC, Wilson PR. Optimal cement space for resin luting cements. Int J Prosthodont 1994; 7:209–15.
- Bagheri R. Film thickness and flow properties of resin-based cements at different temperatures. J Dent 2013; 14:57–63.
- Nawafleh NA, Mack F, Evans J, et al. Accuracy and reliability of methods to measure marginal adaptation of crowns and FDPs: A literature review. J Prosthodont 2013; 22:419–28.
- Sorensen JA. A standardized method for determination of crown margin fidelity. J Prosthet Dent 1990; 64:18–24.
- Lombardo GHL, Nishioka RS, Souza ROA, et al. Influence of surface treatment on the shear bond strength of ceramics fused to cobalt-chromium. J Prosthodont 2010; 19:103–11.
- Strub JR, Rekow ED, Witkowski S. Computer- aided design and fabrication of dental restorations: current systems and future possibilities. J Am Dent Assoc 2006; 137:1289–96.
- Örtorp A, Jönsson D, Mouhsen A, et al. The fit of cobalt-chromium three-unit fixed dental prostheses fabricated with four different techniques: A comparative in vitro study. Dent Mater 2011; 27:356–63.
- van Noort R. The future of dental devices is digital. Dent Mater 2012; 28:3–12.
- Ekren O, Ozkomur A, Ucar Y. Effect of layered manufacturing techniques, alloy powders, and layer thickness on metal-ceramic bond strength. J Prosthet Dent 2018; 119:481–7.
- Sun J, Zhang FQ. The application of rapid prototyping in prosthodontics. J Prosthodont 2012; 21:641–644.
- Santos EC, Shiomi M, Osakada K, et al. Rapid manufacturing of metal components by laser forming. Int J Machine Tools Manufacture 2006; 46:1459-68.
- Kim EH, Lee DH, Kwon SM, et al. A microcomputed tomography evaluation of the marginal fit of cobalt-chromium alloy copings fabricated by new manufacturing techniques and alloy systems. J Prosthetic Dent 2017; 117:393-9.
- Simchi A. Direct laser sintering of metal powders: Mechanism, kinetics and microstructural features. Materials Sci Eng 2006; 428:148-58.
- Sames WJ, List FA, Pannala S, et al. The metallurgy and processing science of metal additive manufacturing. Int Mater Rev 2016; 61:315–60.
- Koutsoukis T, Zinelis S, Eliades G, et al. Selective laser melting technique of Co-Cr dental alloys: A review of structure and properties and comparative analysis with other available techniques. J Prosthod 2015; 24:303-12.
- Bae EJ, Kim JH, Kim WC, et al. Bond and fracture strength of metal-ceramic restorations formed by selective laser sintering. J Adv Prosthod 2014; 6:266-71.
- Papadiochou S, Pissiotis AL. Marginal adaptation and CAD-CAM technology: A systematic review of restorative material and fabrication techniques. J Prosthet Dent 2018; 119:545–51.
- Park JK, Lee WS, Kim HY, et al. Accuracy evaluation of metal copings fabricated by computer-aided milling and direct metal laser sintering systems. J Adv Prosthodont 2015; 7:122.
- James AE, Umamaheswari B, Shanthana Lakshmi CB. Comparative evaluation of marginal accuracy of metal copings fabricated using direct metal laser sintering, computer-aided milling, ringless casting, and traditional casting techniques: An study. Contemp Clin Dent 2018; 9:421–6.
- Kaleli N, Ural Ç, Özköylü G, et al. Effect of layer thickness on the marginal and internal adaptation of laser-sintered metal frameworks. J Prosthet Dent 2019; 121:922–8.
- Koutsoukis T, Zinelis S, Eliades G, et al. Selective laser melting technique of co-cr dental alloys: A review of structure and properties and comparative analysis with other available techniques. J Prosthodont 2015; 24:303–12.
- Mazzoli A. Selective laser sintering in biomedical engineering. Med Biol Eng Comput 2013; 51:245–56.
- Kim KB, Kim WC, Kim HY, et al. An evaluation of marginal fit of three-unit fixed dental prostheses fabricated by direct metal laser sintering system. Dent Mater 2013; 29:e91–6.
- Ahn JS, Lee JH. Comparative evaluation of marginal and internal fit of three-unit Co-Cr frameworks fabricated by metal milling and direct metal laser sintering methods. J Korean Academy Dent Technol 2020; 42:81-9.
- Kim KB, Kim JH, Kim WC, et al. Marginal fit evaluation of 3 unit fixed dental prostheses fabricated by rapid prototyping method. J Korean Academy Dent Technol 2012; 34:105-11.
- Nguyen QB, Luu DN, Nai SM, et al. The role of powder layer thickness on the quality of SLM printed parts. Arch Civil Mechanical Eng 2018; 18:948-55.
- Chockalingam K, Jawahar N, Chandrasekhar U. Influence of layer thickness on mechanical properties in stereolithography. Rapid Prototyping J 2006; 12:106–13.
- Raju BS, Chandrashekar U, Drakshayani DN, et al. Determining the influence of layer thickness for rapid prototyping with stereolithography (SLA) process. Int J Eng Sci Technol 2010; 2:3199–205.
- Sulaiman F, Chai J, Jameson LM, et al. A comparison of the marginal fit of In-Ceram, IPS Empress, and Procera crowns. Int J Prosthodont 1997; 10:478–84.
- Lee JY, Choi SJ, Kim MS, et al. Effect of span length on the fit of zirconia framework fabricated using CAD / CAM system. J Adv Prosthodont 2013; 5:118–25.
- Büchi DL, Ebler S, Hämmerle CHF, et al. Marginal and internal fit of curved anterior CAD/CAM-milled zirconia fixed dental prostheses: An in-vitro study. Quintessence Int 2014; 45:837–46.
- Seelbach P, Brueckel C, Wöstmann B. Accuracy of digital and conventional impression techniques and workflow. Clin Oral Investig 2013; 17:1759–64.
- Ciocca L, Meneghello R, Monaco C, et al. In vitro assessment of the accuracy of digital impressions prepared using a single system for full-arch restorations on implants. Int J Comput Assist Radiol Surg 2018; 13:1097–108.
- Ng J, Ruse D, Wyatt C. A comparison of the marginal fit of crowns fabricated with digital and conventional methods. J Prosthet Dent 2014; 112:555–60.
- Abdel Azim T, Rogers K, Elathamna E, et al. Comparison of the marginal fit of lithium disilicate crowns fabricated with CAD /CAM technology by using conventional impressions and two intraoral digital scanners. J Prosthet Dent 2015; 114:554–559.
Author Info
Harsh Kasabwala1*, Deepak Nallaswamy2 and Subhashree R1
1Department of Prosthodontics, Saveetha Dental College and Hospitals, Saveetha Institute of Medical and Technical Sciences, Saveetha University, Chennai, India2Director of academics, Saveetha Dental College and Hospitals, Saveetha Institute of Medical And Technical Sciences, Saveetha University, Chennai, India
Citation: Harsh Kasabwala, Deepak Nallaswamy, Subhashree R, Influence of Material Layer Deposition Thickness, Span Length of Prosthesis, and type of Laser on the Surface Marginal fit of Different Surfaces of DMLS copings Fabricated using 3 Different DMLS Printing Machines, J Res Med Dent Sci, 2021, 9(11): 147-155
Received: 25-Aug-2021 Accepted: 05-Nov-2021